Samaaro + Your CRM: Zero Integration Fee for Annual Sign-Ups Until 30 June, 2025
- 00Days
- 00Hrs
- 00Min

1
2
3
→
Bottom Line:
without capturing real physician insight, healthcare event marketing reinforces assumptions instead of improving strategy.
Healthcare event marketing generates a constant stream of visible signals. Rooms fill up. Sessions run smoothly. Physicians ask questions, nod along, and stay engaged through discussions. On the surface, it looks like alignment is happening.
It is not.
What you are measuring is behavioral compliance, not cognitive response. Physicians are trained to engage professionally, listen actively, and participate constructively. That behavior creates the appearance of resonance, even when critical evaluation is happening internally.
Most healthcare event dashboards do not capture thinking. They capture movement. They record who showed up, how long they stayed, and whether they interacted. None of that explains what they actually believed, challenged, or rejected.
This is where Insight Blindness begins. You are not missing data. You are interpreting the wrong signals as truth.
The more polished the event, the stronger this illusion becomes.
This blog examines how this illusion forms, where physician thinking disappears, and why it creates a strategic risk for healthcare organizations.

Healthcare marketing decisions are not abstract. They directly influence how therapies are positioned, how education is structured, and how physicians interpret clinical value. These decisions require a precise understanding of medical stakeholder thinking.
Physicians are not passive recipients of information. They evaluate, compare, question, and filter every clinical message they encounter.
Their perspectives shape:
This is not optional context. It is the foundation of an effective strategy.
Healthcare events bring together doctors, experts, and clinical leaders in concentrated settings where particular subjects are thoroughly examined. These times are infrequent. They focus their knowledge and practical experience in one location.
However, the chance is lost if the organization leaves knowing merely who came and how long they stayed.
Without knowing how doctors think, you are left to make decisions regarding their behaviour.
When insight is missing, assumptions take over. Messaging is refined based on internal belief rather than external reality. Campaigns are built on perceived alignment rather than validated understanding.
The risk is not that you know too little. It is that you believe you know enough to act.
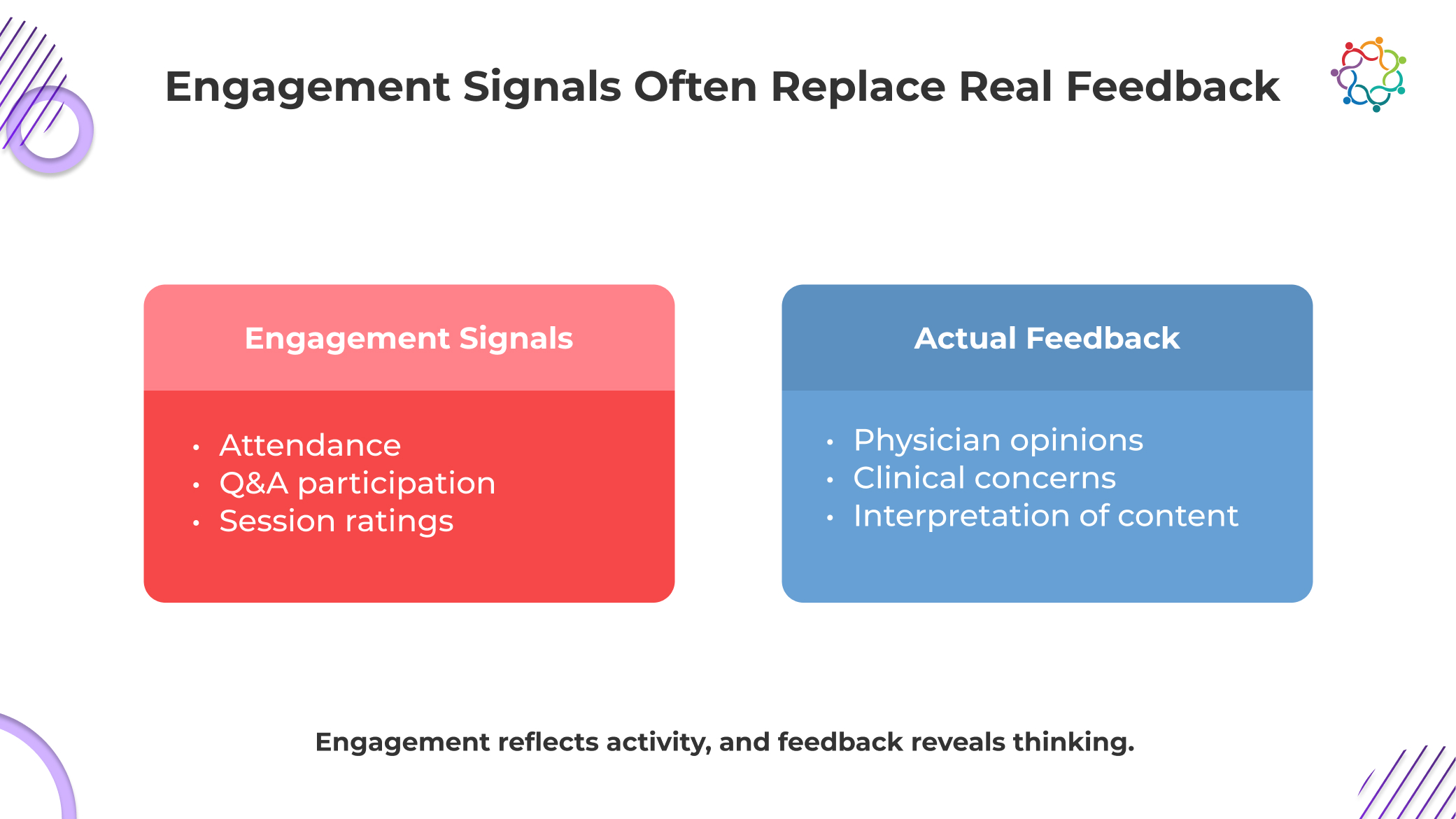
Healthcare event reporting relies on engagement because it is visible, measurable, and easy to present. That convenience creates a problem. These signals do not just lack depth; they distort reality by implying alignment where none may exist.
Full rooms signal topic interest, not message acceptance. Physicians attend to learn and evaluate, not to agree, yet attendance is often misread as endorsement.
Questions indicate engagement with the topic, but often highlight confusion, skepticism, or gaps. Interpreting them as positive validation ignores the intent behind the interaction.
High ratings reflect delivery quality and event organization. They do not confirm whether clinical perspectives were accepted or challenged by the audience.
Active participation can coexist with silent disagreement. Physicians may engage outwardly while internally questioning assumptions, leaving critical perspectives completely unrecorded.
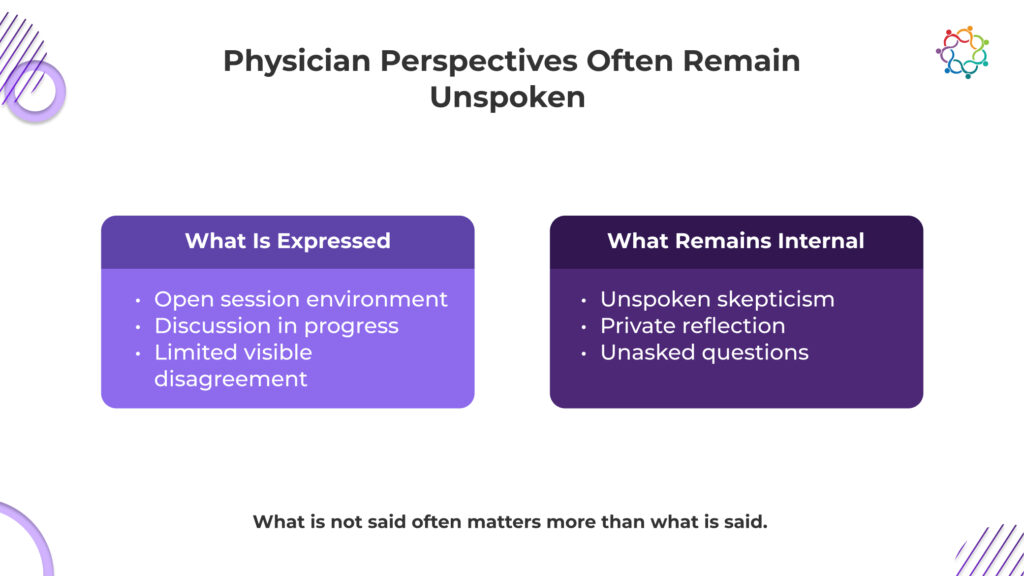
Healthcare settings are subject to limitations that are not present in most marketing scenarios. Physician communication in public is influenced by clinical duty, professional hierarchy, and regulatory sensitivity.
What is said during events is directly impacted by this.
Doctors don’t always publicly question concepts. They don’t always express dissent in front of specialists or their colleagues. They frequently think things through in private, analyse information internally, or talk openly only in casual, trusted contexts.
Silence, in this context, is not neutral. Silence can mean hesitation. It can mean skepticism. It can mean disagreement that is never expressed in the room.
Yet silence is frequently interpreted as acceptance.
This is where Insight Blindness becomes structurally embedded. The environment itself suppresses visible feedback, while the reporting system assumes that visible signals are sufficient. The absence of objection is treated as alignment. The absence of questions is treated as clarity.
Both assumptions are flawed.
Healthcare professionals are trained to evaluate carefully and respond selectively. What they choose not to say publicly is often more important than what they say.
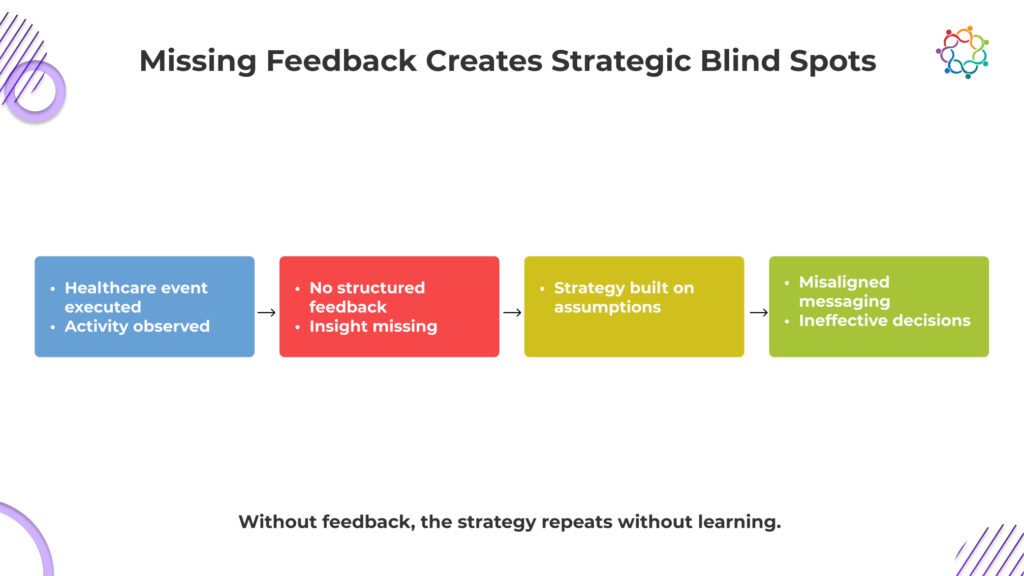
The loss of physician insight does not happen in one obvious moment. It happens across multiple points in the event lifecycle, each one quietly stripping away context that could have informed strategy.
During medical conferences and physician engagement events, the most honest perspectives often emerge outside formal sessions. Hallway discussions, small group conversations, and peer exchanges carry nuanced views that never enter official records.
These conversations reveal hesitation, disagreement, and real-world challenges. Yet they remain invisible to the organization.
Post-event reports are structured around execution. Attendance numbers, session flow, and participation rates dominate the narrative.
This confirms that the event happened successfully. It does not explain what physicians took away from it.
Even when fragments of feedback exist, they are rarely connected. Comments remain isolated. Observations are not synthesized into patterns. No clear view of physician sentiment emerges.
The system captures fragments, not meaning.
What you are left with is a record of activity without interpretation. The event generated signals. The organization failed to translate them into insight.
That is not a data problem. It is a strategic failure.

When healthcare organizations operate without clear visibility into physician thinking, decision-making does not stop. It continues. It simply becomes detached from reality.
This is where Insight Blindness turns into a strategic blind spot.
Marketing teams begin to assume alignment. They interpret engagement as agreement. They believe their clinical positioning resonates because nothing visibly contradicts it.
But physicians may have left the event with:
Without insight into these perspectives, leadership has no way to detect the gap.
You are not operating with partial clarity. You are operating blindly.
The most dangerous part is that the system reinforces itself. Positive metrics validate decisions. Decisions lead to similar events. Similar events produce similar metrics.
At no point is the underlying assumption challenged. This creates a closed loop where strategy is continuously refined without ever being corrected.
Healthcare events are not just engagement platforms. They are concentrated environments of real-world clinical thinking. You bring together physicians who actively treat patients, interpret evidence, and make decisions that directly impact outcomes. That density of perspective is rare.
In these settings, signals emerge constantly. Not in formal sessions, but in reactions, side conversations, hesitation points, and the types of questions that surface. These are early indicators of resistance, confusion, and adoption barriers.
If you are not extracting that, you are not just missing insight. You are actively wasting access to it.
Every event already contains answers to questions your strategy is trying to solve. Why is adoption slow? Where messaging breaks. What physicians do not trust.
If those signals leave the room with the audience, your event delivered activity but retained nothing of strategic value.
When you do not understand the physician’s thinking, the strategy does not pause. It continues, just without correction. That is where the risk compounds.
You repeat messaging because it appeared to work. You scale programs based on engagement signals that never reflect real alignment. You invest more into narratives that may already be breaking down in the minds of physicians.
This is how inefficiency becomes embedded.
Budgets get allocated to reinforce assumptions. Clinical communication drifts away from actual concerns. Opportunities to address skepticism are missed before they are even identified.
The result is not immediate failure. It is slower adoption, weaker influence, and increasing reliance on tactics to compensate for misalignment.
At that point, the issue is no longer execution. It is direction.
You are not optimizing the strategy. You are reinforcing errors with confidence.
Healthcare event marketing continues to expand in scale and sophistication, but the core flaw remains unchanged. It measures what is visible and assumes it reflects what matters. Attendance, engagement, and satisfaction create a convincing story, but not an accurate one.
If you are not capturing how physicians actually think, you are not refining strategy. You are reinforcing assumptions.
This is where most organizations get it wrong. They do not lack data. They lack truth.
And when strategy is built on signals that only look right, healthcare event marketing stops being an advantage.
It becomes a confident, well-funded misdirection.

Samaaro is an AI-powered event marketing platform that enables marketing teams to turn events into a measurable growth channel by planning, promoting, executing, and measuring their business impact.
Location


© 2026 — Samaaro. All Rights Reserved.